
Paul Clare, Managing Director, HSF health plan is shown around the Bio laboratory
On 13th January 2020, Paul Clare and I visited the University of Liverpool to assess a grant application for research into using Melt ElectroWriting (MEW) to treat eye conditions such as glaucoma. The research is supported by the National Eye Research Centre (NERC) and they submitted the grant application.
About The National Eye Research Centre (NERC)
The National Eye Research Centre funds research into the causes and treatments of eye disease, sight loss and blindness. They publish the results of that research in order to stimulate further research advances in ophthalmology. The charity was formed in 1986 and has invested over £14 million into eye research at leading UK centres of excellence in ophthalmology.
Our visit to NERC
I met Laura Serratrice, Chief Executive, NERC, Rachel Williams, Chair in Ocular Biomaterials, University of Liverpool and Dr Lucy Bosworth, Research Fellow. Dr Bosworth gave a presentation about her ground-breaking research into regenerative medicine. Paul and I were also shown some of the scaffolding material and given a comprehensive tour of the Bio laboratory.
Regenerative medicine
Regenerative medicine has enormous potential to treat a multitude of currently incurable conditions – including eye diseases. Technology that allows us to fabricate new tissues to replace those damaged by disease or injury has the power to transform lives – offering real hope to the two million people in the UK who are living with sight loss and a further two million who are predicted to lose their sight by 2050. Coincidentally, HSF has supported a charity called RAFT over a number of years. I have visited RAFT to assess a grant to support tissue reconstruction, which was using the same scaffolding technology as Dr Bosworth.
About Melt ElectroWriting (MEW)
Melt ElectroWriting (MEW) is a new technology, appropriate for regenerative medicine, that manufactures micron-sized* 3D scaffolds, which can be used in tissue engineering to facilitate the growth of cells. To date, this technology has been used to bio-engineer musculoskeletal tissues.
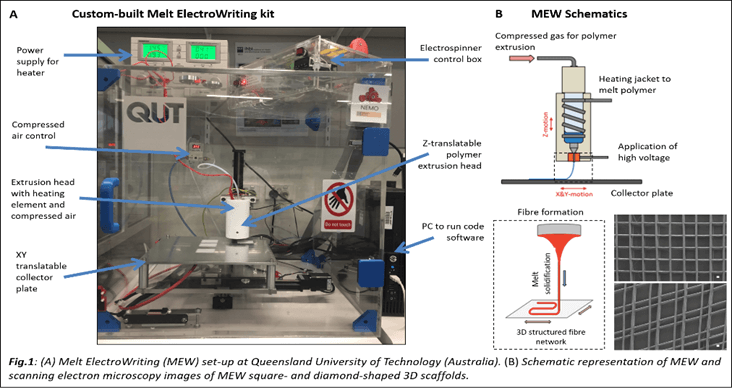
Dr Bosworth is the first person to explore its potential for generating ocular biomaterials that could be used to treat conditions such as glaucoma and age-related macular degeneration, or to repair damaged corneas.
Glaucoma
Glaucoma is the name for a group of eye conditions that cause damage to the optic nerve, leading to vision loss. In most cases, the damage is caused by increased pressure within the eye, resulting from a build-up of fluid called aqueous humour. This fluid is produced in the eye and performs many vital functions including protecting the cornea from disease, dust or pollen. In a healthily functioning eye, the trabecular meshwork helps to maintain normal eye pressure by allowing aqueous humour to drain out of the eye into the vascular system.
Ageing and disease can lead to progressive cell loss, which causes the trabecular meshwork’s sieve-like structure to become blocked, restricting fluid outflow. This causes pressure in the eye to rise, which triggers compression of the optic nerve, resulting in glaucoma.
Currently, there are no regenerative therapies available to treat this condition. MEW will allow the team at Liverpool to fabricate scaffolds with specific dimensions and porosities on which they will grow cells that can be engineered to behave like healthy, functioning trabecular meshwork cells. The ultimate aim will be to implant this cell-loaded scaffold into the eye to restore the fluid outflow pathway.
Using MEW to research Conjunctiva repair
The conjunctiva is a clear, thin membrane that lines the white of the eye and the inside of the eyelids. Its primary function is to keep the front surface of the eye and the inner surfaces of the eyelids moist and lubricated so that the eye can open and close without friction or irritation.
Goblet cells, which are spread throughout the conjunctiva, play a key role in this process. These specialist cells produce mucins – a slimy material that forms part of the tear fluid and provides a protective coating to the outer surface of the eye. Mucins are spread evenly over the eye’s surface by eyelid movement during blinking.
The conjunctiva is susceptible to damage from disease and traumas caused by chemical burns or side effects from contact with medications (e.g. glaucoma medication). Scarring and prolonged inflammation of the conjunctiva can lead to persistent discomfort, ocular surface failure, and corneal disease.
Transplants can be used to treat corneal disease but only if the conjunctiva is healthy and at present, there is no reliable method for replacing and restoring the conjunctiva. Dr Bosworth has been amazed by how the stability of the MEW scaffolding has led to healthy Goblet cell growth producing large amounts of mucins.
It is hoped, that eventually, MEW technology might be used to produce a full cornea which could be used for medical research.
Looking ahead
NERC are looking to raise £20K towards MEW equipment which will be brought from Brisbane in Australia. We look forward to further updates from NERC on using Melt ElectroWriting (MEW) to treat eye conditions.
To learn more about NERC, please visit their website: https://www.nercuk.org/









Comments are closed.